| Pornpat Hengudomsub | 2 Articles |
Purpose
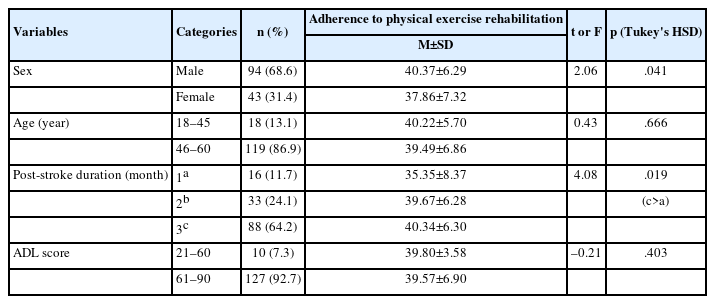
This study aimed to identify key predictive factors influencing adherence to physical exercise rehabilitation among adults during the first three months following a first-onset ischemic stroke in China. Methods: A cross-sectional descriptive study was conducted among 137 adults who attended clinical follow-up appointments within the first three months after experiencing a first-onset ischemic stroke. Predictors included family support, coping with role transition, depression, self-efficacy, and body image. Hierarchical multiple regression analysis was performed. Results: The mean adherence score for physical exercise rehabilitation was 39.58 (standard deviation=6.71), indicating a moderate adherence level (70.6%). In model 1, male sex (β=.20, p=.017) and post-stroke duration of 2 months (β=.31, p=.015) and 3 months (β=.39, p=.002) were significant predictors of adherence to physical exercise rehabilitation. Adding main predictors in model 2 resulted in a significant increase in explained variance (ΔR²=.418, p<.001), accounting for 51.5% of the total variance (R²=.515, adjusted R²=.484). Male sex (β=.15, p=.017), family support (β=.43, p<.001), self-efficacy (β=.26, p<.001), depression (β=–.24, p=.001), and coping with role transition (β=.16, p=.033) were significant predictors. Body image and post-stroke duration were not significant after adjustment. Conclusion: Efforts to promote adherence to physical exercise rehabilitation should prioritize family support, depressive symptoms, self-efficacy, and coping with role transition. Furthermore, body image may warrant attention when developing sex-specific intervention strategies.
Purpose
This study aimed to identify predictors of quality of life (QoL), including self-efficacy, social support, illness perceptions, and resilience, among colorectal cancer patients during the first 1 to 6 months after stoma surgery. Methods A predictive correlational design was used with 142 adult patients who had undergone stoma surgery within the preceding 1 to 6 months. Data were collected using validated instruments measuring QoL, self-efficacy, social support, illness perceptions, and resilience. The data were analyzed using descriptive statistics, the independent t-test, one-way analysis of variance, the Games-Howell post-hoc test, Pearson correlation coefficients, and hierarchical multiple linear regression analysis. Results The participants had a mean age of 56.15 years (standard deviation, 6.51 years); 67.6% were male, and 57.0% had a temporary stoma. In model 1, the method of paying medical expenses significantly predicted QoL, explaining 6.0% of the variance (adjusted R²=.06, p=.006), with self-financed patients reporting lower QoL than insured patients. In model 2, the addition of psychosocial variables (self-efficacy, social support, illness perceptions, and resilience) substantially improved the model, explaining 70.0% of the variance (adjusted R²=.70, p<.001). In the final model, illness perceptions (β=−.61), social support (β=.32), resilience (β=.20), and self-efficacy (β=.19) were significant predictors (all p<.001), whereas method of paying medical expenses was no longer significant. Conclusion This study provides evidence to support the development of interventions targeting illness perceptions, social support, resilience, and self-efficacy to improve QoL among stoma patients during the early postoperative period.
|
|

