| Chutima Chantamit-O-Pas | 2 Articles |
Purpose
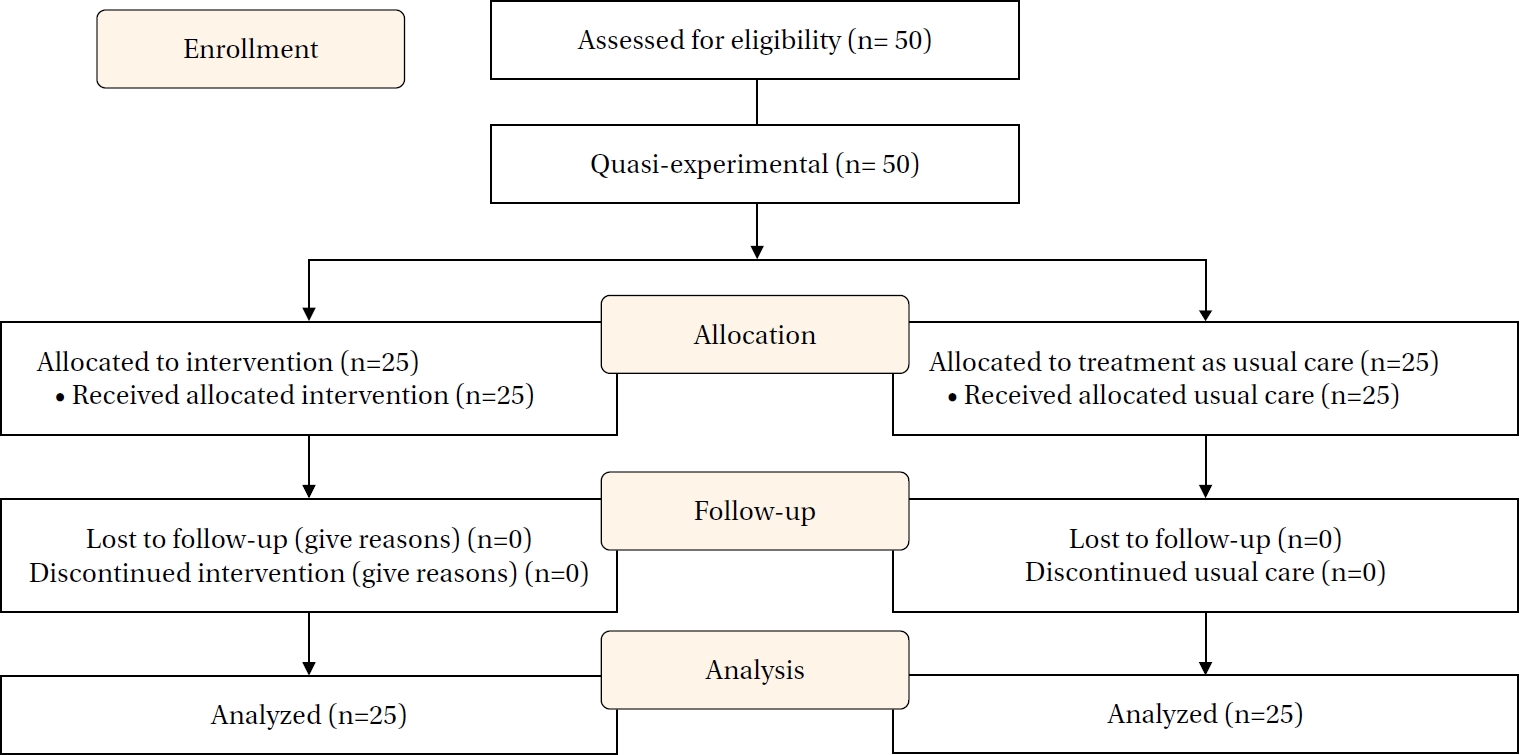
Stage 3 chronic kidney disease (CKD) is highly prevalent and often progresses to end-stage renal disease without effective self-management. This study examined the effects of an Individual and Family Self-Management Program delivered via a mobile communication application on self-management behaviors and clinical outcomes among patients with stage 3 CKD. Methods A 12-week quasi-experimental study with a pretest-posttest control group design was conducted among 50 patients with stage 3 CKD at a tertiary hospital in Thailand, between January and May 2024. The intervention group received a self-management program grounded in Individual and Family Self-Management Theory and delivered via the LINE chatbot. The program included educational content, self-regulation strategies, and structured family support, while the control group received usual care. Outcomes included self-management behaviors, estimated glomerular filtration rate (eGFR), systolic blood pressure (SBP), diastolic blood pressure (DBP), and hemoglobin A1c (HbA1c). Analysis of covariance was used to adjust for baseline differences. Results After adjustment for baseline values, the intervention group showed significantly greater improvements in self-management behaviors (F=7.92, p<.05) and eGFR (F=52.92, p<.001) compared with the control group. Significant reductions were also observed in SBP (F=26.84, p<.001), DBP (F=12.61, p<.05), and HbA1c levels (F=7.74, p<.05). Conclusion A mobile-based Individual and Family Self-Management Program effectively improved self-management behaviors and key clinical outcomes among patients with stage 3 CKD, supporting the integration of family engagement and digital technology in chronic disease care.
Purpose
This study aimed to identify predictors of quality of life (QoL), including self-efficacy, social support, illness perceptions, and resilience, among colorectal cancer patients during the first 1 to 6 months after stoma surgery. Methods A predictive correlational design was used with 142 adult patients who had undergone stoma surgery within the preceding 1 to 6 months. Data were collected using validated instruments measuring QoL, self-efficacy, social support, illness perceptions, and resilience. The data were analyzed using descriptive statistics, the independent t-test, one-way analysis of variance, the Games-Howell post-hoc test, Pearson correlation coefficients, and hierarchical multiple linear regression analysis. Results The participants had a mean age of 56.15 years (standard deviation, 6.51 years); 67.6% were male, and 57.0% had a temporary stoma. In model 1, the method of paying medical expenses significantly predicted QoL, explaining 6.0% of the variance (adjusted R²=.06, p=.006), with self-financed patients reporting lower QoL than insured patients. In model 2, the addition of psychosocial variables (self-efficacy, social support, illness perceptions, and resilience) substantially improved the model, explaining 70.0% of the variance (adjusted R²=.70, p<.001). In the final model, illness perceptions (β=−.61), social support (β=.32), resilience (β=.20), and self-efficacy (β=.19) were significant predictors (all p<.001), whereas method of paying medical expenses was no longer significant. Conclusion This study provides evidence to support the development of interventions targeting illness perceptions, social support, resilience, and self-efficacy to improve QoL among stoma patients during the early postoperative period.
|
|

